It starts with an itch. Not just any itch, but a deep, persistent urge to scratch that feels impossible to ignore. For millions of people living with atopic dermatitis, also known as eczema, this sensation is the enemy. It disrupts sleep, ruins clothes, and damages the skin’s protective layer, creating a vicious cycle of inflammation and pain.
You might wonder why some days your skin is calm while others are on fire. The truth is, atopic dermatitis isn't just a surface-level rash; it's a complex condition rooted in genetics and immune system dysregulation. But here is the good news: you have more control than you think. By understanding what triggers your flares and mastering the art of emollient therapy, you can significantly reduce symptoms and improve your quality of life.
The Root Cause: Why Your Skin Barrier Fails
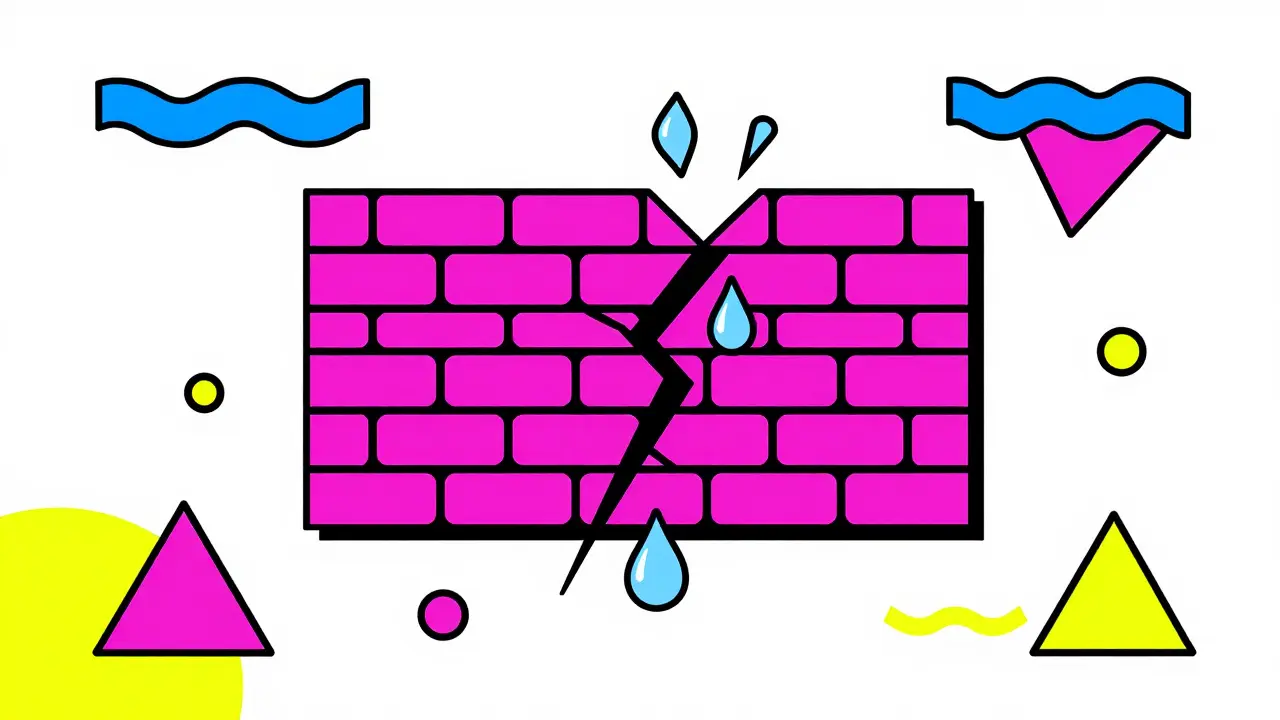
To manage atopic dermatitis effectively, you first need to understand what is happening beneath the surface. Think of healthy skin like a brick wall. The bricks are skin cells, and the mortar holding them together is made of lipids, including ceramides, cholesterol, and fatty acids. In people with atopic dermatitis, this "mortar" is defective or missing.
This defect often stems from genetic mutations. Approximately 15-50% of patients with moderate-to-severe atopic dermatitis have mutations in the filaggrin gene. Filaggrin is a protein crucial for maintaining hydration and structural integrity in the outermost layer of the skin. Without enough functional filaggrin, your skin cannot retain moisture effectively.
The result? Increased transepidermal water loss (TEWL). While healthy skin loses about 5-10 grams of water per square meter per hour, skin affected by atopic dermatitis can lose 15-30 grams. This dryness makes the skin vulnerable to irritants, allergens, and microbes, triggering the immune system to overreact. This inflammatory response causes the redness, swelling, and intense itching characteristic of flare-ups.
Identifying Your Personal Flare Triggers
If the skin barrier is broken, environmental factors easily slip through and cause trouble. However, triggers vary widely from person to person. What sets off one patient might not affect another. Here are the most common culprits backed by clinical data:
- Humidity and Temperature: Cold, dry air is a major enemy. When humidity drops below 40%, the risk of flares increases by 37%. Conversely, heat above 80°F (27°C) triggers flares in 68% of patients because sweat contains salts and proteins that irritate compromised skin.
- Irritants in Cleansers: Harsh soaps strip away natural oils. Sodium lauryl sulfate, found in many body washes, can cause significant barrier disruption even at concentrations as low as 0.5%.
- Fragrances: About 15% of patients experience flares directly linked to fragrances in lotions, detergents, or personal care products. These chemical compounds are frequent sensitizers.
- Stress: Psychological stress activates the nervous system, which can release neuropeptides that exacerbate inflammation and itching.
- Microbes: Staphylococcus aureus colonizes the skin of up to 90% of atopic dermatitis patients during flares, compared to less than 5% in healthy individuals. This bacteria releases toxins that worsen inflammation.
Keep a symptom diary for two weeks. Note what you ate, wore, and touched before each flare. Patterns will emerge, helping you avoid specific triggers unique to your biology.
Emollient Therapy: The Cornerstone of Management
Medications like topical corticosteroids treat the inflammation, but they do not fix the underlying barrier defect. That is where emollients come in. They are not just moisturizers; they are medical devices designed to restore the skin barrier. According to the American Academy of Dermatology (AAD), emollient therapy is the first-line treatment for all patients, regardless of severity.
Emollients work through three main mechanisms:
- Occlusion: Ingredients like petrolatum create a physical barrier on top of the skin, preventing water loss. Petrolatum has a 98% efficacy rate in reducing TEWL.
- Humectancy: Agents like glycerin attract water from the deeper layers of the skin and the environment into the stratum corneum. Optimal concentrations range from 40-50%.
- Emolliency: Lipids like ceramides fill the gaps between skin cells, repairing the "mortar" of the skin barrier. Ceramides are most effective at concentrations of 0.5-3%.
Research shows that consistent emollient use reduces flares by 36% over six months. More importantly, it has an excellent safety profile. Adverse events occur in only 2.3% of users, compared to 15-20% for topical corticosteroids. This makes emollients safe for long-term daily use, even on sensitive areas like the face.

Choosing the Right Formulation
Not all creams are created equal. The texture and ingredient list matter immensely. Here is how to choose wisely:
| Type | Key Ingredients | Best For | Pros | Cons |
|---|---|---|---|---|
| Ointments | Petrolatum | Severe dryness, nighttime use | Highest occlusivity, fewest preservatives | Greasy feel, stains clothing |
| Creams | Ceramides, Glycerin | Daily maintenance, daytime use | Balanced hydration, non-greasy | May contain preservatives |
| Lotions | Glycerin, Light oils | Mild cases, large body areas | Easy to spread, fast absorption | Lower efficacy, higher alcohol content |
Avoid products with fragrance, dyes, or harsh preservatives like methylisothiazolinone, which caused contact dermatitis in 5.7% of emollient users in recent studies. Look for labels stating "fragrance-free" rather than "unscented," as unscented products may still contain masking agents.
The "Soak and Seal" Method
Applying emollients correctly is just as important as choosing the right product. Many patients apply too little or at the wrong time. Dr. Amy Paller from Northwestern University emphasizes that timing is critical: applying emollients within three minutes of bathing locks in 50% more moisture.
Follow these steps for optimal results:
- Bathe Briefly: Take a lukewarm bath or shower for 15-20 minutes. Avoid hot water, which strips natural oils.
- Use Gentle Cleansers: Use a soap-free, syndet bar or liquid cleanser only on dirty areas like armpits and groin. Rinse thoroughly.
- Pat Dry: Gently pat your skin with a soft towel until it is slightly damp. Do not rub.
- Apply Immediately: Within three minutes, apply a thick layer of emollient. Use downward strokes to minimize irritation.
- Reapply Throughout the Day: Apply again at least once more during the day, especially after washing hands.
How much should you use? The AAD recommends 250-500 grams per week for adults and 500-1000 grams for children. This sounds like a lot, but remember that you are replacing lost lipids. Using less than 50 grams weekly has been shown to result in 43% more flares.

When Emollients Aren't Enough
While emollients are foundational, they are not a cure-all for severe cases. If your skin remains inflamed despite rigorous emollient use, you likely need adjunctive therapies. Topical corticosteroids remain the gold standard for acute flares, achieving clearance in 70-80% of mild-to-moderate cases when combined with emollients.
For sensitive areas like the face or eyelids, topical calcineurin inhibitors like tacrolimus or pimecrolimus are preferred because they do not cause skin thinning. In recent years, biologic agents like dupilumab have revolutionized treatment for moderate-to-severe atopic dermatitis, reducing flares by 70-80% by targeting specific immune pathways.
However, never stop using emollients when starting other medications. They work synergistically. As Dr. Eric Simpson notes, "Without consistent barrier repair, no other treatment can be fully effective." Emollients prepare the skin to absorb topical medications better and protect against the side effects of stronger drugs.
Overcoming Common Barriers
We know the science works, yet adherence remains low. Only 35% of patients maintain consistent emollient use after six months. Why? Mostly due to "greasiness" and the perceived burden of application.
To overcome this, try switching formulations based on the season. Use heavier ointments in winter and lighter creams in summer. Set reminders on your phone to apply lotion twice daily. Involve family members in the routine, especially for children. Education is key-understanding that emollients are medicine, not just cosmetics, helps shift mindset.
Cost is another factor. Prescription-grade emollients can cost $20-$40 monthly. However, consider the alternative: frequent doctor visits, steroid prescriptions, and missed work or school days due to flares. Investing in high-quality, fragrance-free emollients is a cost-effective strategy for long-term management.
Can I use Vaseline for atopic dermatitis?
Yes, Vaseline (petrolatum) is highly effective for atopic dermatitis. It is an occlusive agent that creates a strong barrier against water loss. It is inexpensive, fragrance-free, and hypoallergenic. However, it can feel greasy and stain clothes, so it is best used at night or on very dry patches.
How often should I apply emollients?
You should apply emollients at least twice daily. Ideally, apply immediately after bathing and then again later in the day. If your skin feels tight or itchy, reapply more frequently. Consistency is more important than the amount applied at one time.
Are natural oils like coconut oil good for eczema?
Natural oils can be helpful for some, but they are not standardized. Coconut oil has antimicrobial properties and may help with Staphylococcus aureus colonization. However, some natural oils can act as allergens. It is safer to use medically formulated emollients with known ingredients like ceramides and petrolatum.
Why does my skin itch more after applying lotion?
If your skin itches more after application, you may be reacting to an ingredient such as fragrance, preservatives, or lanolin. Switch to a plain petrolatum-based ointment or a fragrance-free cream with minimal ingredients. Also, ensure you are applying the lotion to damp skin, as applying to very dry skin can sometimes sting.
Do I need to continue using emollients if my skin looks clear?
Yes, absolutely. Atopic dermatitis is a chronic condition involving a permanent skin barrier defect. Even when your skin looks clear, the barrier remains fragile. Continuing emollient therapy prevents future flares and maintains skin health. Think of it like brushing your teeth-you don't stop because your teeth aren't currently hurting.