When your muscles suddenly feel heavy, and simple tasks like climbing stairs or lifting a coffee cup become exhausting, it’s easy to blame aging or laziness. But for some people, this isn’t fatigue-it’s muscle inflammation from a rare autoimmune condition. Dermatomyositis and polymyositis are two closely related diseases that attack the body’s own muscle tissue, leaving patients weak, frustrated, and often misdiagnosed. Unlike temporary soreness from exercise, this inflammation doesn’t go away with rest. It demands medical attention, precise diagnosis, and a long-term treatment plan.
What Exactly Are Dermatomyositis and Polymyositis?
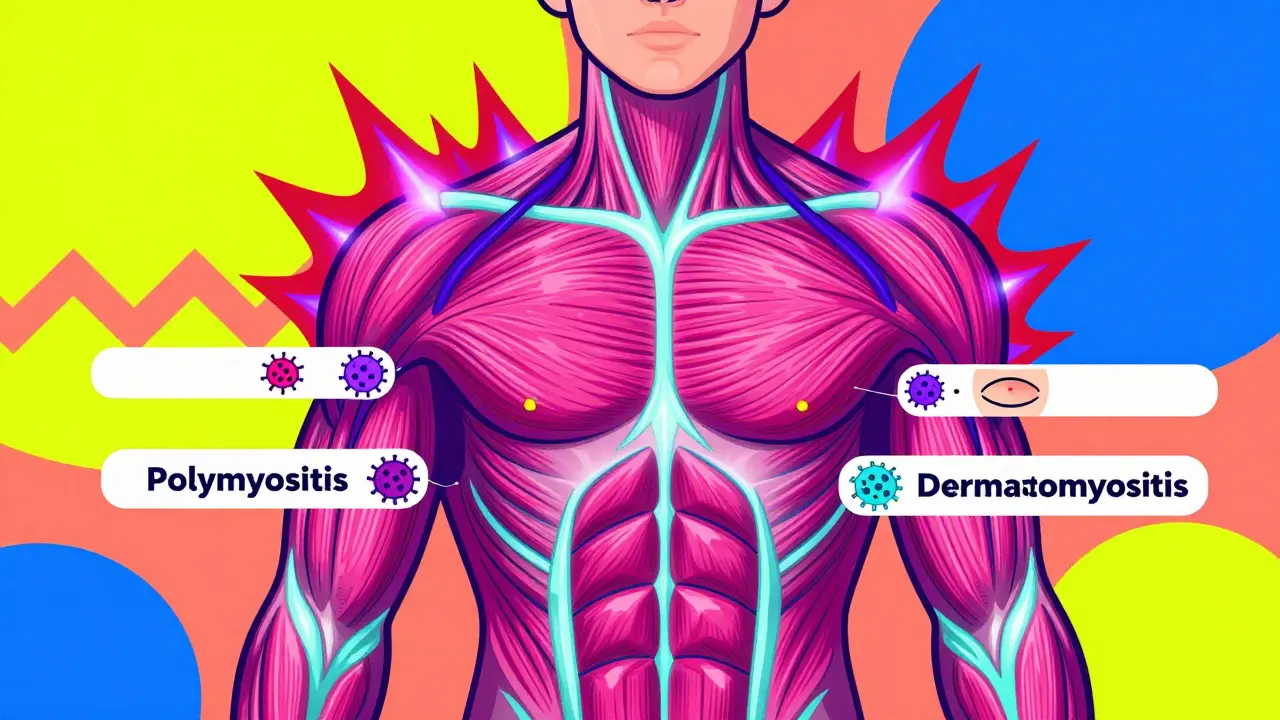
Both conditions fall under the umbrella of inflammatory myopathies, meaning they cause chronic inflammation in skeletal muscles. Polymyositis (PM) affects muscles without skin involvement, while dermatomyositis (DM) adds distinctive rashes to the picture. These aren’t just different names for the same thing-they’re separate diseases with different causes, symptoms, and risks. Polymyositis typically shows up in adults between 30 and 60, with women two to three times more likely to be affected than men. The weakness starts slowly, usually in the muscles closest to the trunk: hips, thighs, shoulders, and neck. You might notice trouble standing up from a chair, lifting your arms above your head, or even swallowing. There’s no pain, just deep, persistent fatigue. Dermatomyositis shares those muscle symptoms but adds visible signs. The hallmark is the heliotrope rash-a purplish-red discoloration on the eyelids that looks like a sunburn you didn’t earn. You’ll also see red, scaly patches over knuckles, elbows, knees, and the neck. In kids, these rashes can appear as bumpy, raised spots on the fingers. These skin changes aren’t cosmetic-they’re warning signs that the immune system is targeting muscle tissue.Why Do These Conditions Happen?
These aren’t caused by infection, injury, or overuse. They’re autoimmune disorders. That means your immune system, which should protect you, turns against your own body. The trigger? No one knows for sure. Genetics may play a role, and some cases follow viral infections or cancer, but no single cause has been pinned down. The big difference between the two lies in how the immune system attacks. In polymyositis, T cells invade muscle fibers directly, destroying them from within. In dermatomyositis, it’s more about B cells and antibodies that attack blood vessels around the muscle, cutting off oxygen and nutrients. This is why skin and lung problems are common in DM but rare in PM.How Are They Diagnosed?
Misdiagnosis is shockingly common. About 30% of patients see multiple doctors over years before getting the right answer. Many are told they have fibromyalgia, lupus, or even thyroid issues because the symptoms overlap. But accurate diagnosis requires more than just feeling weak. The process usually starts with blood tests. Creatine phosphokinase (CPK) levels are often five to ten times higher than normal. Normal CPK is 10-120 U/L; in active disease, it can hit 8,000 or more. Other markers like ESR and CRP show inflammation, and ANA (antinuclear antibodies) are frequently positive. Next comes electromyography (EMG), which checks how muscles respond to nerve signals. In these diseases, EMG shows short, low-amplitude electrical bursts and spontaneous firing-signs of damaged muscle tissue. Imaging helps too. MRI scans can highlight inflamed areas in muscles, guiding where to take a biopsy. And yes, the gold standard is still the muscle biopsy. In polymyositis, you’ll see immune cells clustered around non-dead muscle fibers. In dermatomyositis, the telltale sign is perifascicular atrophy-muscle fibers at the edges of bundles are dying while the center stays intact.What Makes Dermatomyositis Different?
Dermatomyositis carries extra risks that polymyositis doesn’t. About 20% of adults with DM are diagnosed with cancer within five years of their muscle symptoms starting. The most common links are ovarian, lung, breast, and gastrointestinal cancers. That’s why doctors run full cancer screenings-chest X-rays, abdominal ultrasounds, mammograms, colonoscopies-at diagnosis. Lung involvement is also more common in DM. Between 30% and 40% develop interstitial lung disease, which causes shortness of breath and dry cough. This can be more dangerous than the muscle weakness itself. Regular lung function tests are part of routine care. There’s also a pediatric version of dermatomyositis, with peaks around ages 5-15. Kids often get calcium deposits under the skin (calcinosis) and more severe GI symptoms. Their treatment approach differs slightly from adults.
How Is It Treated?
There’s no cure. But with the right treatment, most people regain strength and live full lives. The goal isn’t to eliminate the disease-it’s to control it before it causes permanent damage. Corticosteroids like prednisone are the first step. Doctors usually start with 1 mg per kilogram of body weight daily-roughly 40-60 mg for most adults. This is aggressive, but it’s needed to stop the immune system from tearing up muscles. After 4-8 weeks, the dose is slowly lowered. The problem? Long-term steroids cause bone loss, weight gain, diabetes, and cataracts. About half of patients on long-term steroids develop osteoporosis. That’s why second-line drugs kick in. Methotrexate, azathioprine, and mycophenolate mofetil are immunosuppressants that help reduce steroid doses. One patient on Reddit shared that adding methotrexate dropped their CPK from 8,200 to 450 in four months, letting them cut their steroid dose by 75%. For tough cases, especially in dermatomyositis, IVIG (intravenous immunoglobulin) is used. It’s a concentrated mix of antibodies from donors that helps calm the immune system. Studies show it works well for skin rashes and muscle weakness when other drugs fail. Newer options are emerging. JAK inhibitors like tofacitinib, originally for rheumatoid arthritis, are now showing promise in dermatomyositis. A 2023 trial found 65% improvement in skin scores and over 50% improvement in muscle strength. Another drug, abatacept, is being tested for polymyositis and has shown early success in reducing disease activity.Physical Therapy Is Not Optional
Medicines stop the attack. But rebuilding strength? That’s up to you-and physical therapy. Starting exercise within two weeks of diagnosis is critical. Too much too soon can make things worse, but too little leads to permanent atrophy. The right program is low-resistance, high-repetition: leg lifts, arm curls, walking, swimming. It’s not about lifting heavy weights. It’s about keeping muscles alive. Studies show patients who stick with structured rehab improve functional capacity by 35-45% in six months. One survey found 74% of patients who did physical therapy regained the ability to climb stairs and rise from chairs without help.What About Side Effects?
Treatment isn’t easy. Steroids cause weight gain in 82% of patients who experience side effects. Insomnia, mood swings, and thinning skin are common. Many report feeling like they’re losing themselves to the meds. That’s why monitoring is part of care. Bone density scans every year. Blood sugar checks. Eye exams. Calcium and vitamin D supplements. Your doctor should talk to you about these risks before starting treatment. Swallowing problems affect 15-30% of patients. If food or liquid goes down the wrong pipe, it can lead to pneumonia. Speech therapists help with swallowing techniques and diet changes-like switching to softer foods or thickened liquids.Prognosis Has Improved Dramatically
Twenty years ago, survival rates for these diseases were around 50-60%. Today, with early diagnosis and modern drugs, 10-year survival exceeds 80% for dermatomyositis and 85% for polymyositis. The key? Getting treated within the first six months of symptoms. One study found that patients who started treatment early had an 80% chance of reaching remission or low disease activity. Those who waited over a year had much lower success rates.Living With the Condition
This isn’t a disease you can cure and forget. It’s managed, day after day. Patients often need regular blood tests, doctor visits, and adjustments to their meds. Some go years without flare-ups. Others have relapses triggered by stress, infection, or sun exposure. Sun protection is crucial for dermatomyositis. UV light can worsen rashes and trigger flares. Broad-spectrum sunscreen, hats, and avoiding midday sun aren’t optional-they’re medical advice. Support matters too. The Myositis Association reports that 68% of patients struggle with fatigue that limits daily life. Talking to others who get it-through forums, support groups, or online communities-makes a real difference.Why This Matters
These are rare diseases. Only 1-10 people per 100,000 are diagnosed each year. That means most doctors won’t see a case in their entire career. But that doesn’t mean they’re unimportant. They’re complex, treatable, and often misunderstood. If you’ve been told your weakness is "just aging," or your fatigue is "all in your head," get a second opinion. Ask for a rheumatologist. Push for blood tests. Demand a biopsy if needed. You don’t have to live with unexplained muscle weakness. Treatment works. Recovery is possible. And with the right care, you can get back to the things that matter-walking, lifting, breathing, living.Can dermatomyositis and polymyositis be cured?
No, there is no known cure for either condition. However, with early and aggressive treatment, most patients can achieve remission or low disease activity. This means symptoms are controlled, muscle strength improves, and damage is prevented. The goal of treatment is long-term management, not permanent elimination of the disease.
How long does it take to diagnose these conditions?
On average, diagnosis takes 3 to 6 months from the first symptom. Many patients see multiple doctors and undergo several tests before getting a correct diagnosis. Misdiagnosis is common, occurring in about 30% of cases, often mistaken for fibromyalgia, lupus, or thyroid disorders. Early referral to a rheumatologist and timely muscle biopsy can shorten this timeline significantly.
Are these conditions hereditary?
They are not directly inherited, but genetics may increase susceptibility. People with certain immune system genes are more likely to develop these conditions, especially if triggered by environmental factors like infections or sun exposure. No single gene causes the disease, but family history of autoimmune disorders can raise risk.
Why is cancer screening important in dermatomyositis?
About 20% of adults with dermatomyositis develop cancer within five years of diagnosis, especially ovarian, lung, breast, or gastrointestinal cancers. The immune system’s attack on muscle tissue may be triggered by an underlying tumor. That’s why full cancer screening-including imaging and blood tests-is standard practice at diagnosis. Polymyositis does not carry the same cancer risk.
Can children get dermatomyositis?
Yes, dermatomyositis has a pediatric form, with peaks between ages 5 and 15. Children often have more severe skin rashes, calcium deposits under the skin (calcinosis), and gastrointestinal issues. Treatment is similar to adults but requires special monitoring for growth and bone health. Polymyositis does not occur in children.
What role does physical therapy play in treatment?
Physical therapy is essential. Medications stop the immune attack, but therapy rebuilds muscle strength and prevents permanent atrophy. Low-resistance exercises-like walking, swimming, and light resistance training-improve function by 35-45% within six months. Starting within two weeks of diagnosis gives the best results. Avoiding exercise can lead to irreversible muscle loss.
What are the biggest side effects of steroid treatment?
Long-term steroid use causes osteoporosis (in 30-50% of patients), weight gain (reported by 82% of those with side effects), diabetes (15-30% risk), cataracts (20-40%), and mood changes. Doctors manage these with calcium and vitamin D supplements, bone density scans, blood sugar monitoring, and by reducing steroid doses as soon as possible using other immunosuppressants.
Is there a new treatment on the horizon?
Yes. JAK inhibitors like tofacitinib have shown strong results in refractory dermatomyositis, improving both skin and muscle symptoms in clinical trials. Abatacept is being tested for polymyositis and has shown promise in early studies. These drugs target specific parts of the immune system, offering hope for more effective, less toxic treatments in the near future.

February 25, 2026 AT 13:05 PM
man i wish i knew this stuff when my aunt was going through this. they told her it was just fibromyalgia for two years. she lost so much muscle mass before they finally did the biopsy. now she’s on methotrexate and doing way better, but she’ll never get back full strength in her legs. physical therapy saved her. don’t wait like we did.
February 27, 2026 AT 02:27 AM
Just wanted to add that sun exposure can totally trigger a flare in DM. My dermatologist made me buy SPF 50+ daily sunscreen and wear wide-brimmed hats even on cloudy days. It’s not optional. I used to think it was overkill until I got a bad rash after a weekend at the lake. Now I never skip it.
February 27, 2026 AT 08:17 AM
As someone from India, I’ve seen so many cases go undiagnosed because families assume muscle weakness is just aging or ‘nervous exhaustion.’ We need more awareness here. My cousin was misdiagnosed for 18 months - her CPK was over 9,000 by the time they tested. Please, if you’re in a region with limited access to rheumatologists, push for bloodwork. It’s cheap. It matters.
February 28, 2026 AT 06:59 AM
IVIG is wild. I had a friend who couldn’t lift a fork, and after two rounds of IVIG, she started cooking again. Not a cure, but a lifeline. Also, the cost is insane here - like $15k per infusion. Insurance fights it every time. If you’re lucky enough to get it covered, don’t waste it.
February 28, 2026 AT 17:20 PM
They don’t tell you how much your personality changes on steroids. I went from chill to screaming at my dog for breathing too loud. My husband left. I didn’t blame him. The weight gain, the mood swings - it’s like your body becomes a stranger. And then you’re told to ‘just exercise.’ Like that’s gonna fix the emotional wreckage.
March 1, 2026 AT 12:10 PM
There’s a deeper philosophical layer here that rarely gets discussed. These conditions force us to confront the fragility of autonomy. The body, once a vessel of agency, becomes a battleground. We are not just treating muscles - we are negotiating with an immune system that has turned traitor. The tragedy isn’t just the weakness - it’s the erosion of trust in one’s own physiology. Recovery isn’t merely physical; it’s existential.
March 2, 2026 AT 05:55 AM
Let’s talk about JAK inhibitors. I’m not a doc, but I’ve been following the trials. Tofacitinib isn’t magic - but for my cousin, it was the first thing that made her rash fade without crushing her with steroids. It’s not FDA-approved for DM yet, but off-label use is happening. Ask your rheum if they’ve considered it. Don’t wait for the textbook to catch up.
March 3, 2026 AT 09:08 AM
Let’s be real - the ‘85% survival rate’ sounds great, but it’s not the whole story. What about the 15% who die from lung fibrosis? Or the ones who end up in wheelchairs despite ‘early treatment’? And don’t even get me started on the financial ruin from lifelong meds and PT. This isn’t a feel-good story. It’s a slow burn.
March 3, 2026 AT 12:38 PM
Okay but like… why is this even a thing? Why does the body do this? Like, what’s the evolutionary advantage of turning on your own muscles? Did we evolve to be weak? Was this some ancient survival mechanism that backfired? I feel like we’re just patching symptoms and not asking the real question - why is my immune system so pissed off at me?
March 4, 2026 AT 16:08 PM
I’ve been living with DM for 7 years. I’m not ‘cured’ - but I can hike now. I can carry groceries. I can lift my kid. It took years. The steroids wrecked my hips. The PT hurt. But I did it. If you’re reading this and you’re scared - I get it. But don’t give up. There’s life after diagnosis. It’s different. But it’s still yours.
March 5, 2026 AT 11:24 AM
Actually, the 20% cancer link in dermatomyositis is misleading. Most studies are retrospective and selection-biased. The real incidence is closer to 8-10%, and many of those cancers are caught early because of the screening - not because DM causes cancer. It’s a correlation, not causation. The fearmongering around cancer screening is doing more harm than good - unnecessary biopsies, anxiety, financial toxicity. We need better risk stratification, not blanket panic.