If you've ever told a doctor you have a "sulfa allergy," you might be accidentally blocking yourself from getting the best possible treatment for your blood pressure, glaucoma, or joint pain. For decades, the medical world has used the term "sulfa" as a catch-all, leading millions of people to believe that any drug containing a sulfur-based molecule is dangerous for them. But here is the reality: having a reaction to a sulfa antibiotic doesn't mean you're allergic to every drug with "sulfa" in the name.
The confusion stems from a massive gap between how we label these drugs and how they actually behave in your body. Many people find themselves in a frustrating loop where a pharmacy flag prevents them from taking a necessary diuretic or a common painkiller, simply because of a vague note in their medical file. Understanding the difference between antimicrobial and non-antimicrobial sulfonamides is the key to unlocking safer, more effective healthcare.
The Big Misconception: Not All Sulfas Are Equal
When people talk about a sulfa drug allergy is a hypersensitivity reaction to sulfonamide-containing medications, most commonly the antibiotic variety, they are usually talking about a specific group of medicines. The term "sulfa" is shorthand for sulfonamides. While thousands of compounds contain sulfur, only a small subset are actually problematic for people with these allergies.
Research shows a stark contrast between reported allergies and confirmed ones. While about 3% of the population reports a sulfa allergy, a study by Macy et al. in 2019 found that only 1.5% to 2% actually have a confirmed IgE-mediated reaction. The rest are often experiencing non-allergic side effects or are reacting to a different drug entirely. This creates a "documentation burden" where electronic health records are cluttered with warnings that aren't clinically relevant, leading to unnecessary medication swaps.
Why Do Some Sulfa Drugs React While Others Don't?
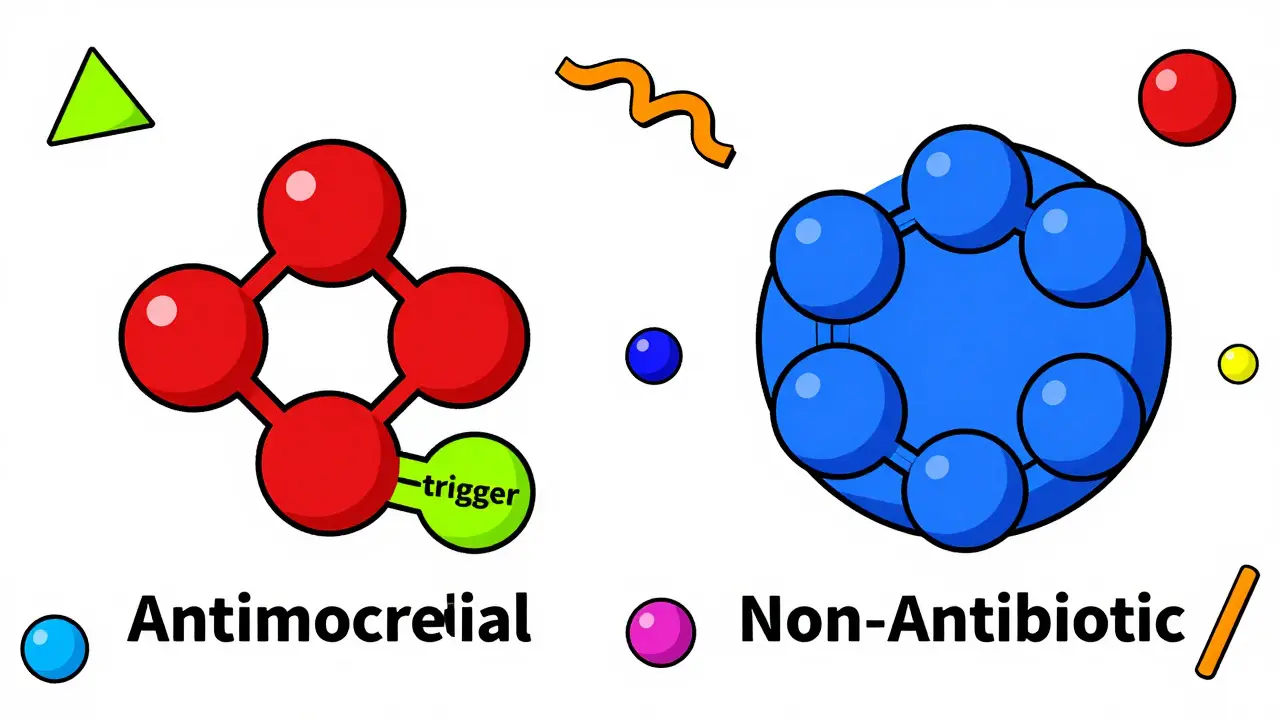
It all comes down to the molecular architecture. It isn't the sulfur atom itself that causes the allergic reaction; it's a specific structure called the arylamine group (an aromatic amine at the N4 position). In antimicrobial sulfonamides, this group is metabolized into hydroxylamine, a reactive compound that can bind to proteins in your system and trigger an immune response.
Non-antibiotic sulfonamides simply don't have this specific "trigger" structure. Because they lack the arylamine group, your immune system doesn't recognize them as the same threat. This is why someone can have a severe reaction to a sulfa antibiotic but take a sulfa-based blood pressure medication for twenty years without a single sneeze or rash.
| Feature | Antimicrobial Sulfonamides | Non-Antibiotic Sulfonamides |
|---|---|---|
| Core Structure | Contains Arylamine Group | Lacks Arylamine Group |
| Common Examples | Sulfamethoxazole, Sulfadiazine | Furosemide, Celecoxib, HCTZ |
| Reaction Risk | High cross-reactivity within class | Negligible risk for sulfa-allergic patients |
| Primary Use | Bacterial Infections (UTIs) | Hypertension, Edema, Pain |
Which Medications Should You Actually Avoid?
If you have a confirmed sulfonamide antibiotic allergy, you need to be careful with drugs that share that specific chemical trigger. The most common culprits include Sulfamethoxazole (often found in Bactrim or Septra), sulfadiazine, and sulfacetamide. Dapsone is another one to watch, as it shares structural similarities and can trigger a reaction.
There is one notable outlier: Sulfasalazine. Used often for inflammatory bowel disease or rheumatoid arthritis, it is partially metabolized into sulfapyridine, which is an antimicrobial sulfonamide. Because of this, about 10% of people with a sulfa antibiotic allergy will react to it. Most other non-antibiotic versions are safe.
On the flip side, you can generally stop worrying about these common medications unless you have a separate, specific allergy to them:
- Diuretics: Furosemide (Lasix) and Hydrochlorothiazide (HCTZ).
- NSAIDs: Celecoxib (Celebrex). In a multi-center trial of 450 patients, less than 0.5% of sulfa-allergic people reacted to this drug.
- Diabetes Meds: Sulfonylureas like glyburide.
- Daily items: Sulfites in wine, sulfates in Epsom salts, and saccharin in artificial sweeteners. These do not have the arylamine group and are safe.
The Danger of the "Sulfa Label"
When a patient is labeled with a generic "sulfa allergy," it often leads to a domino effect of poor medical decisions. In hospitals, this often results in "antibiotic selection errors." Instead of using a targeted sulfonamide, doctors might prescribe a broader-spectrum drug like a fluoroquinolone. While these work, they carry a higher risk of causing C. difficile infections-a dangerous gut bacteria that can lead to severe colitis.
The economic impact is also staggering. The Agency for Healthcare Research and Quality estimated in 2023 that inappropriate restrictions on these drugs cost the US healthcare system about $1.2 billion annually due to more expensive alternative medications and longer hospital stays. More importantly, patients suffer. Many report being denied life-saving heart failure medications like furosemide simply because a computer screen flagged a "sulfa" warning.

How to Manage Your Allergy Labels Moving Forward
The best way to ensure you get the right care is to move away from vague terminology. If you have a reaction to a sulfa drug, don't just say "I'm allergic to sulfa." Instead, use the phrase "sulfonamide antibiotic allergy." This one small change in wording tells the provider exactly which chemical structure is the problem, leaving the door open for safe use of non-antibiotic sulfonamides.
If you've had a mild reaction in the past-like a slight rash without any swelling or trouble breathing-you might actually be fine with non-antibiotic sulfonamides. Some specialists suggest a "single-therapeutic-dose challenge," where you take a small dose under medical supervision to see if a reaction occurs. In a 2019 study, 98.7% of patients with a history of sulfa antibiotic allergy successfully tolerated hydrochlorothiazide during such a challenge.
However, if you have ever experienced severe reactions like Stevens-Johnson Syndrome (SJS) or Toxic Epidermal Necrolysis (TEN)-conditions where the skin blisters and peels-you must avoid antimicrobial sulfonamides for life. Even in these extreme cases, non-antibiotic sulfonamides are usually still a safe option, but this should always be managed by an allergist.
Can I take Celebrex if I have a sulfa allergy?
Yes, in most cases. Major medical organizations, including the American College of Rheumatology, state that there is no clinically significant cross-reactivity between sulfonamide antibiotics and Celecoxib. The risk of a reaction is roughly the same as it is for the general population.
Are Epsom salts and wine safe for people with sulfa allergies?
Yes. Sulfates (found in Epsom salts) and sulfites (found in wine) are completely different from sulfonamides. They lack the arylamine group that triggers the allergic reaction, so they do not cause cross-reactivity.
What is the difference between a side effect and a true sulfa allergy?
A true allergy is an immune response, often involving IgE antibodies, which can cause hives, swelling, or anaphylaxis. A side effect (or adverse reaction) might be nausea or a mild stomach ache. Many people are labeled "allergic" when they actually just experienced a non-allergic side effect.
Why do some doctors still tell me to avoid all sulfa drugs?
Medical education often lags behind current research. A 2023 survey found that 67% of primary care physicians still believe non-antibiotic sulfonamides should be avoided, despite expert consensus and large-scale studies proving they are safe.
What should I do if my medical record says "Sulfa Allergy"?
Ask your doctor to clarify the label. Request that they change "Sulfa Allergy" to "Sulfonamide Antibiotic Allergy" if that's what you actually reacted to. This prevents you from being denied necessary medications like diuretics or certain pain relievers in the future.
Next Steps for Patients and Caregivers
If you are currently avoiding medications due to a "sulfa allergy" label, your first step should be a conversation with a pharmacist or an allergist. They can help you determine if your reaction was to an antimicrobial or a non-antimicrobial drug. If you have a history of severe skin reactions, do not attempt a medication challenge at home; always do so in a clinical setting.
For those managing chronic conditions like hypertension or heart failure, ensure your care team understands the distinction between drug classes. This prevents the use of less effective alternatives and reduces the risk of complications from over-prescribing broad-spectrum antibiotics. Accurate documentation is not just about paperwork-it's about getting the right drug for the right reason.


